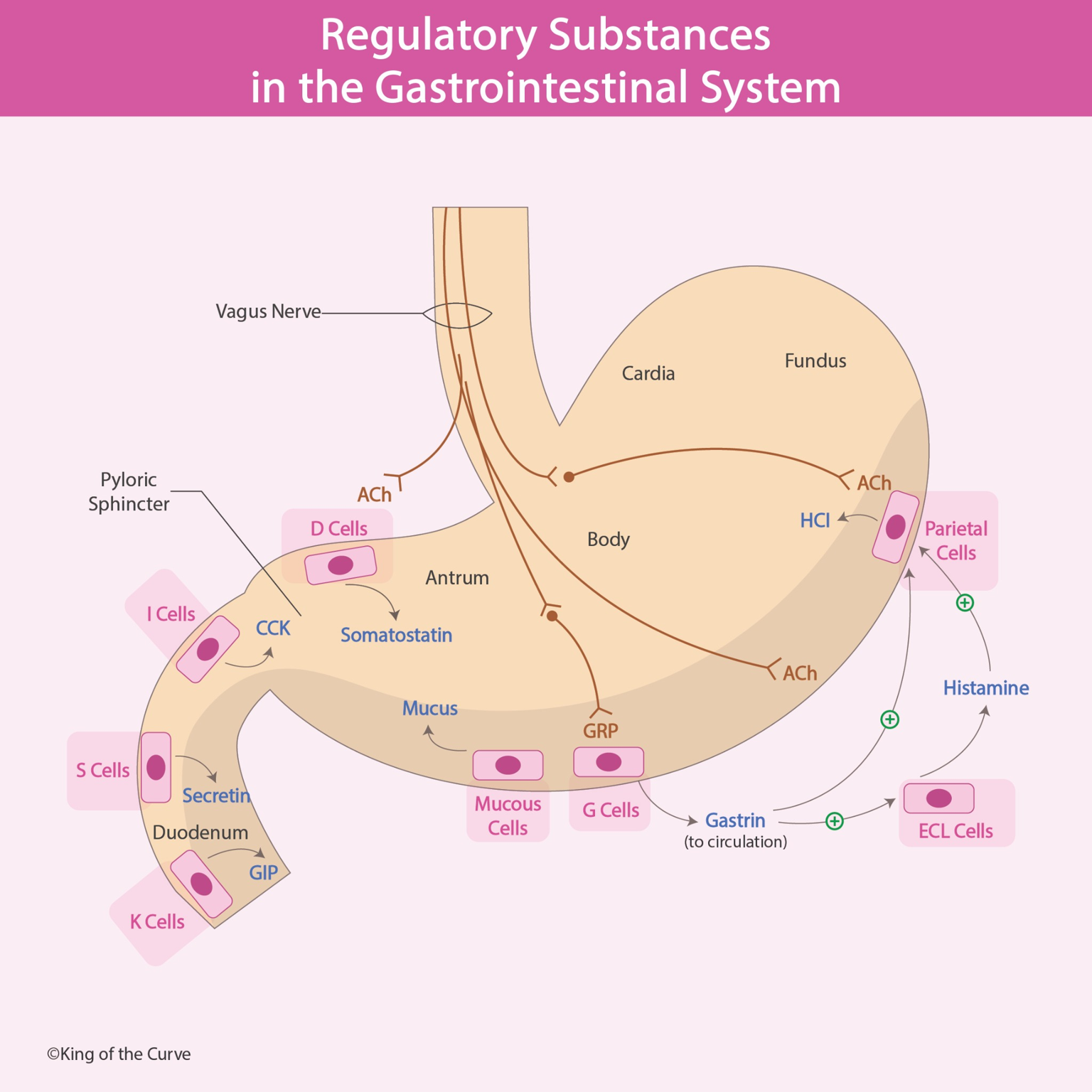
🧠 Regulatory Substances in the Gastrointestinal System
The gastrointestinal (GI) system is regulated by a complex network of neural, hormonal, and paracrine mediators. These substances coordinate acid secretion, enzyme release, motility, and mucosal protection. A delicate balance between stimulatory and inhibitory signals ensures effective digestion while preventing tissue injury.
🧵 Neural Regulation: The Vagus Nerve
The vagus nerve provides parasympathetic stimulation to the stomach through the release of acetylcholine (ACh).
ACh directly stimulates:
Parietal cells → increased HCl secretion
ECL cells → histamine release
Mucus cells → enhanced mucosal protection
Additionally, the vagus releases gastrin-releasing peptide (GRP), which stimulates G cells to secrete gastrin. This makes vagal input one of the most powerful upstream regulators of gastric acid secretion.
🧪 Gastrin: The Hormonal Driver
G cells located in the antrum release gastrin into the bloodstream in response to food intake and vagal stimulation.
Gastrin:
Directly stimulates parietal cells
Stimulates ECL cells to release histamine
Promotes gastric mucosal growth
Because it acts via circulation, gastrin is classified as a hormone. Excess production can lead to acid hypersecretion disorders such as Zollinger–Ellison syndrome.
🔥 Histamine: The Potent Amplifier
Enterochromaffin-like (ECL) cells release histamine in response to gastrin and acetylcholine.
Histamine binds to H₂ receptors on parietal cells, activating the Gs pathway and increasing cAMP. This strongly enhances acid secretion.
Histamine acts locally, making it a paracrine mediator that amplifies other stimulatory signals.
🛑 Somatostatin: The Master Brake
D cells secrete somatostatin, the primary inhibitory regulator of gastric acid secretion.
Somatostatin:
Inhibits gastrin release
Inhibits histamine release
Directly suppresses parietal cell activity
It serves as a negative feedback mechanism when gastric pH becomes too low, protecting the mucosa from excessive acid exposure.
🌊 Secretin: The Acid Neutralizer
S cells in the duodenum release secretin in response to acidic chyme entering from the stomach.
Secretin:
Stimulates pancreatic bicarbonate secretion
Reduces gastric acid secretion
Slows gastric emptying
Its primary function is to protect the small intestine and optimize pH for digestive enzymes.
🥑 Cholecystokinin (CCK): The Fat Regulator
I cells release CCK in response to fats and amino acids.
CCK:
Stimulates pancreatic enzyme secretion
Causes gallbladder contraction
Slows gastric emptying
Modulates acid secretion indirectly
It coordinates digestion of fats and proteins while preventing excessive gastric activity.
🍬 Gastric Inhibitory Peptide (GIP)
K cells secrete GIP when glucose and fats enter the small intestine.
GIP:
Stimulates insulin release (incretin effect)
Decreases gastric acid secretion
Slows gastric motility
It links nutrient absorption with endocrine regulation of metabolism.
📊 Summary Table: Regulatory Substances in the GI System
| Substance | Cell Source | Type | Primary Target | Second Messenger | Effect on Acid Secretion | Additional Functions |
|---|---|---|---|---|---|---|
| Acetylcholine (ACh) | Vagus nerve | Neural | M3 receptor (parietal cell) | ↑ IP3 / ↑ Ca2+ | Stimulates | Stimulates histamine release |
| Gastrin | G cells (antrum) | Hormone | CCKB receptor | ↑ IP3 / ↑ Ca2+ | Stimulates | Mucosal growth, ↑ histamine |
| Histamine | ECL cells | Paracrine | H2 receptor | ↑ cAMP | Strongly stimulates | Amplifies ACh & gastrin |
| Somatostatin | D cells | Paracrine | SST receptor | ↓ cAMP | Inhibits | Inhibits gastrin & histamine |
| Secretin | S cells (duodenum) | Hormone | Pancreas, stomach | ↓ acid activity | Inhibits | ↑ bicarbonate secretion |
| CCK | I cells (duodenum) | Hormone | Pancreas, gallbladder | Ca2+ mediated | Indirect modulation | ↑ enzymes, ↓ gastric emptying |
| GIP | K cells (duodenum) | Hormone | Pancreas, stomach | ↑ cAMP (β-cells) | Inhibits | ↑ insulin (incretin effect) |
⚖️ Integration of Signals
The stomach integrates multiple overlapping pathways:
Stimulatory mediators:
ACh, gastrin, histamine
Inhibitory mediators:
Somatostatin, secretin, GIP
Protective mechanisms:
Mucus and bicarbonate secretion
All stimulatory signals ultimately converge at the H⁺/K⁺-ATPase proton pump, the final common pathway for acid secretion.
🏥 Clinical Relevance
Disruption of these regulatory systems can contribute to:
Peptic ulcer disease
GERD
Gastrinoma (Zollinger–Ellison syndrome)
NSAID-induced gastric injury
Many therapies target these pathways, including proton pump inhibitors (PPIs), H₂ receptor blockers, and somatostatin analogs.
Frequently Asked Questions (FAQs)
-
Aim for 4-6 focused hours, ensuring you incorporate breaks to avoid burnout.
-
Practice mindfulness techniques, take practice exams under realistic conditions, and maintain a balanced lifestyle.
-
Set short-term goals, seek support from mentors, and reward yourself for small achievements.
-
Regular exercise improves focus, reduces stress, and enhances overall mental clarity.
-
KOTC offers personalized learning tools, gamification features, and adaptive question banks to help students stay on track without burnout.