🩸 Heparin-Induced Thrombocytopenia (HIT): Mechanism, Risks & Management
Heparin-Induced Thrombocytopenia (HIT) is a serious immune-mediated complication of heparin therapy. Although it causes a low platelet count, paradoxically, it increases the risk of dangerous blood clots (thrombosis).
🔍 What Is HIT?
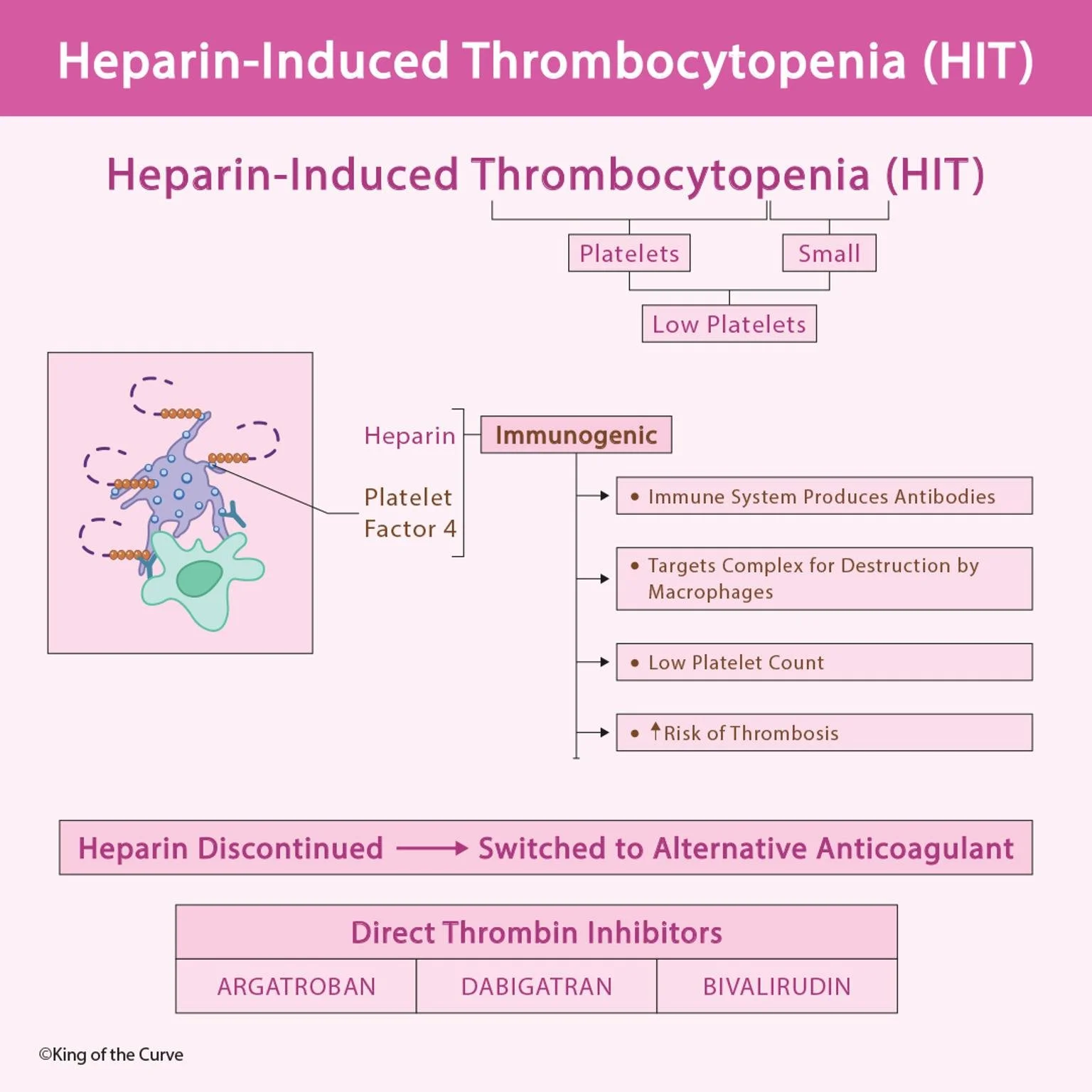
HIT is an immune reaction that occurs when heparin binds to a protein released by platelets called Platelet Factor 4 (PF4).
This complex becomes immunogenic, triggering the immune system to produce antibodies.
⚙️ Pathophysiology of HIT
🧬 Step-by-Step Mechanism:
Heparin binds to Platelet Factor 4 (PF4)
The complex becomes immunogenic
The immune system produces IgG antibodies
Antibodies bind to the heparin–PF4 complex
This activates platelets → platelet consumption
Platelets are destroyed by macrophages → low platelet count
⚠️ Why Is HIT Dangerous?
Despite causing thrombocytopenia (low platelets), HIT leads to:
🔥 Increased risk of thrombosis (clot formation)
🧠 Stroke
🫀 Myocardial infarction
🦵 Deep vein thrombosis (DVT)
🫁 Pulmonary embolism (PE)
👉 This happens because activated platelets promote clot formation.
📉 Key Features of HIT
Platelet count drops significantly
Typically occurs 5–10 days after heparin exposure
Can occur earlier if previously exposed to heparin
Associated with paradoxical clotting, not bleeding
🧪 Diagnosis
HIT is suspected clinically and confirmed with lab tests:
🧾 4T Score (clinical probability tool)
🧪 PF4 antibody ELISA
⚡ Serotonin release assay (gold standard)
🚫 Management of HIT
❗ Immediate Action:
Stop heparin immediately
🔄 Switch to Alternative Anticoagulants:
💊 Direct Thrombin Inhibitors:
Argatroban
Dabigatran
Bivalirudin
👉 These drugs prevent clot formation without triggering HIT
⚠️ Important Clinical Tip
❌ Never give warfarin alone in acute HIT
✔️ It can worsen thrombosis and cause complications like skin necrosis
📊 Summary Table
| Feature | Description |
|---|---|
| Cause | Immune reaction to heparin–PF4 complex |
| Platelets | Decreased |
| Risk | Increased thrombosis |
| Onset | 5–10 days after exposure |
| Treatment | Stop heparin + start alternative anticoagulant |
🧠 Key Takeaways
HIT is immune-mediated, not just a drug side effect
Causes low platelets but high clot risk
Early recognition is life-saving
Treatment requires immediate heparin discontinuation
Frequently Asked Questions (FAQs)
-
Aim for 4-6 focused hours, ensuring you incorporate breaks to avoid burnout.
-
Practice mindfulness techniques, take practice exams under realistic conditions, and maintain a balanced lifestyle.
-
Set short-term goals, seek support from mentors, and reward yourself for small achievements.
-
Regular exercise improves focus, reduces stress, and enhances overall mental clarity.
-
KOTC offers personalized learning tools, gamification features, and adaptive question banks to help students stay on track without burnout.