🧠 Distal Convoluted Tubule (DCT): Function and Pharmacology
The Distal Convoluted Tubule (DCT) is an important segment of the nephron responsible for fine-tuning electrolyte balance, particularly sodium and calcium. Located after the loop of Henle, the DCT plays a crucial role in regulating Na⁺ reabsorption, Ca²⁺ handling, and overall fluid balance, making it a key target for certain diuretics.
⚙️ Sodium and Chloride Handling
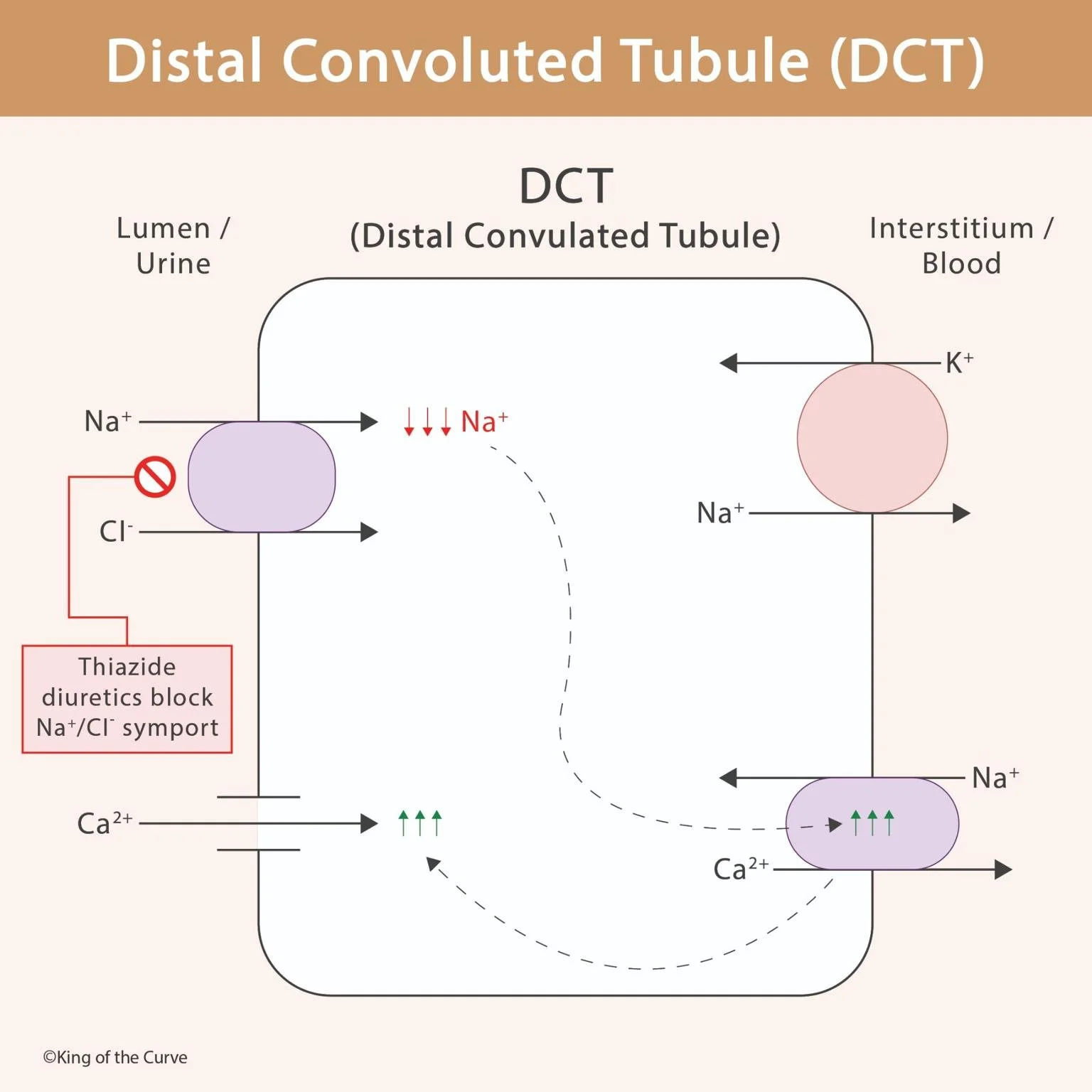
In the DCT, sodium (Na⁺) and chloride (Cl⁻) are reabsorbed from the tubular lumen into the epithelial cells via the Na⁺/Cl⁻ symporter located on the apical membrane. This process is essential for maintaining sodium balance and contributes to extracellular fluid volume.
Once inside the cell, sodium is actively transported into the bloodstream by the Na⁺/K⁺ ATPase pump on the basolateral membrane, while potassium (K⁺) moves into the cell. This pump maintains the electrochemical gradient that drives sodium entry from the lumen.
💊 Thiazide Diuretics: Mechanism of Action
The DCT is the primary site of action of thiazide diuretics. These drugs block the Na⁺/Cl⁻ symporter, reducing sodium reabsorption. As a result, more sodium (and water) remains in the urine, producing a diuretic effect.
Clinically, thiazides are widely used in:
Hypertension
Edema
Calcium-related kidney stones
🦴 Calcium Reabsorption in the DCT
One of the unique features of the DCT is its role in calcium (Ca²⁺) reabsorption. Calcium enters the epithelial cell from the lumen through channels on the apical membrane and is then transported into the bloodstream via a Na⁺/Ca²⁺ exchanger on the basolateral side.
Interestingly, when thiazide diuretics inhibit sodium reabsorption, intracellular sodium levels decrease. This enhances the activity of the Na⁺/Ca²⁺ exchanger, leading to increased calcium reabsorption. This is why thiazides can reduce urinary calcium excretion.
🔁 Integrated Transport Mechanisms
The coordinated function of transporters in the DCT ensures efficient electrolyte balance:
Na⁺/Cl⁻ symporter → brings Na⁺ and Cl⁻ into the cell
Na⁺/K⁺ ATPase → pumps Na⁺ into blood, maintains gradient
Na⁺/Ca²⁺ exchanger → promotes Ca²⁺ reabsorption
These mechanisms work together to regulate blood pressure, electrolyte levels, and fluid homeostasis.
📊 Clinical Correlation
Dysfunction or pharmacologic manipulation of the DCT can have significant clinical effects:
Thiazide use → decreased Na⁺ reabsorption, increased Ca²⁺ reabsorption
Hypokalemia → due to downstream effects in the collecting duct
Hypercalcemia (mild) → due to increased Ca²⁺ retention
Understanding DCT physiology is essential for interpreting electrolyte abnormalities and managing conditions like hypertension and kidney stones.
📊 Key Transporters and Their Functions in the DCT
| Component | Location | Function | Clinical Relevance |
|---|---|---|---|
| Na+/Cl− Symporter | Apical membrane | Reabsorbs Na+ and Cl− from lumen | Blocked by thiazide diuretics |
| Na+/K+ ATPase | Basolateral membrane | Pumps Na+ into blood and K+ into cell | Maintains gradient for Na+ reabsorption |
| Ca2+ Channel | Apical membrane | Allows Ca2+ entry into the cell | Regulated by parathyroid hormone (PTH) |
| Na+/Ca2+ Exchanger | Basolateral membrane | Moves Ca2+ into blood in exchange for Na+ | Enhanced with thiazide use |
📌 Regulation of DCT Function
The activity of the distal convoluted tubule is tightly regulated by hormones and physiological needs. Parathyroid hormone (PTH) plays a major role by increasing calcium reabsorption in the DCT, which is especially important in maintaining serum calcium levels. Additionally, subtle changes in sodium delivery to the DCT can influence downstream segments like the collecting duct, affecting potassium and hydrogen ion secretion.
The DCT also contributes to long-term blood pressure control. By adjusting sodium reabsorption, it indirectly influences extracellular fluid volume. This is why medications targeting the DCT, such as thiazide diuretics, are first-line treatments in hypertension—they reduce plasma volume and decrease peripheral resistance over time.
Frequently Asked Questions (FAQs)
-
Aim for 4-6 focused hours, ensuring you incorporate breaks to avoid burnout.
-
Practice mindfulness techniques, take practice exams under realistic conditions, and maintain a balanced lifestyle.
-
Set short-term goals, seek support from mentors, and reward yourself for small achievements.
-
Regular exercise improves focus, reduces stress, and enhances overall mental clarity.
-
KOTC offers personalized learning tools, gamification features, and adaptive question banks to help students stay on track without burnout.