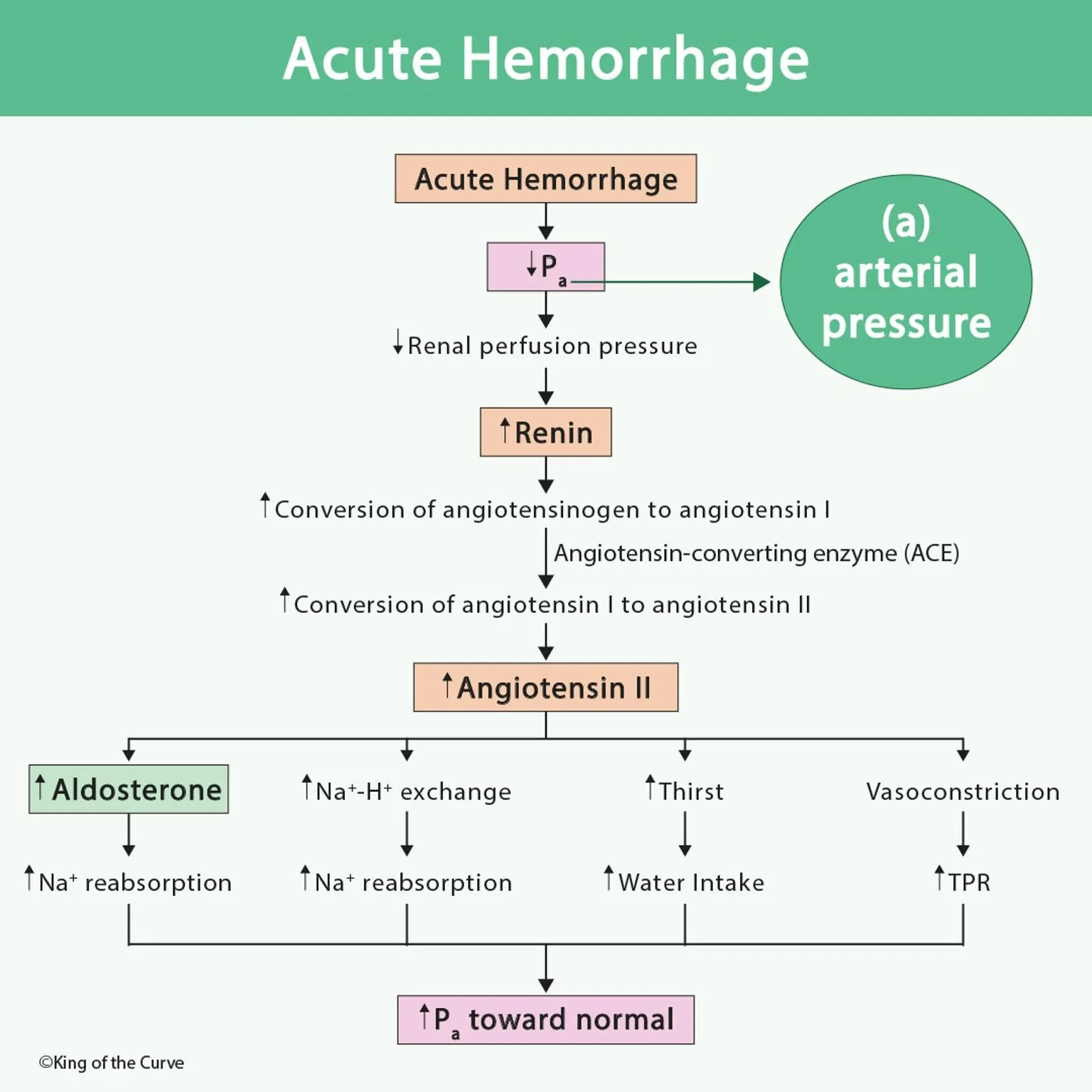
🩸 Acute Hemorrhage and the RAAS Response
Acute hemorrhage refers to a sudden loss of blood volume, which leads to a rapid decrease in arterial pressure. This drop in blood pressure compromises organ perfusion, particularly affecting the kidneys. To counteract this life-threatening situation, the body activates several compensatory mechanisms, the most important being the Renin-Angiotensin-Aldosterone System (RAAS).
🔍 Step-by-Step Mechanism
1. ↓ Arterial Pressure (Pa)
Acute hemorrhage causes a decrease in arterial pressure, reducing blood flow to vital organs.
2. ↓ Renal Perfusion Pressure
The kidneys detect reduced perfusion pressure, especially at the juxtaglomerular apparatus, which acts as a sensor for blood pressure changes.
3. ↑ Renin Release
In response, the kidneys release renin, an enzyme that initiates the RAAS cascade.
⚙️ Activation of the RAAS Pathway
Renin converts angiotensinogen (produced by the liver) into angiotensin I, which is then converted into angiotensin II by angiotensin-converting enzyme (ACE) in the lungs.
Effects of Angiotensin II:
↑ Aldosterone secretion (adrenal cortex)
↑ Sodium (Na⁺) reabsorption
↑ Na⁺–H⁺ exchange in kidneys
↑ Thirst → Increased water intake
Vasoconstriction → ↑ Total Peripheral Resistance (TPR)
⚠️ Role of the Sympathetic Nervous System
In addition to RAAS activation, acute hemorrhage also stimulates the sympathetic nervous system (SNS). Baroreceptors in the carotid sinus and aortic arch detect the drop in arterial pressure and trigger increased sympathetic output. This leads to tachycardia, increased cardiac contractility, and peripheral vasoconstriction, all of which help maintain blood flow to vital organs such as the brain and heart. The SNS response acts rapidly and works synergistically with RAAS to stabilize circulation during acute blood loss.
💉 Importance of Timely Intervention
While the body’s compensatory mechanisms are effective in the short term, they are often insufficient in cases of severe hemorrhage. Without prompt medical intervention—such as fluid resuscitation, blood transfusion, and control of the bleeding source—prolonged hypoperfusion can lead to shock, organ failure, and death. Early recognition and treatment are therefore critical to improving patient outcomes and preventing complications associated with sustained low blood pressure.
📊 Summary Table
| Component | Effect | Outcome |
|---|---|---|
| Renin | Activates RAAS | Starts BP recovery |
| Angiotensin II | Vasoconstriction | ↑ TPR → ↑ Blood Pressure |
| Aldosterone | ↑ Na⁺ reabsorption | ↑ Blood volume |
| Thirst | ↑ Water intake | Restores fluid balance |
| Na⁺–H⁺ Exchange | ↑ Sodium retention | Supports volume expansion |
🧠 Clinical Insight
The RAAS system is a powerful compensatory mechanism, but excessive or prolonged activation can be harmful. Chronic activation is seen in conditions like heart failure, hypertension, and renal artery stenosis, where it contributes to fluid overload and increased vascular resistance. This is why medications such as ACE inhibitors, ARBs, and aldosterone antagonists are commonly used to block different parts of this pathway.
🩺 Key Takeaway
In acute hemorrhage, the body rapidly activates the RAAS system to restore arterial pressure. Through a combination of vasoconstriction, sodium retention, and increased water intake, blood pressure is brought back toward normal, helping preserve vital organ function.
Frequently Asked Questions (FAQs)
-
Aim for 4-6 focused hours, ensuring you incorporate breaks to avoid burnout.
-
Practice mindfulness techniques, take practice exams under realistic conditions, and maintain a balanced lifestyle.
-
Set short-term goals, seek support from mentors, and reward yourself for small achievements.
-
Regular exercise improves focus, reduces stress, and enhances overall mental clarity.
-
KOTC offers personalized learning tools, gamification features, and adaptive question banks to help students stay on track without burnout.